at a glance
Is Myoinositol Safe to Take in a PCOS Pregnancy?
Table of Contents
- 01 - What is PCOS?
- 02 - What is insulin and why is it important to understand in the context of Polycystic Ovarian Syndrome?
- 03 - Your Ovary Doesn't Become Insulin Resistant
- 04 - What is myoinositol?
- 05 - Secondary insulin messengers, the ovary, and PCOS
- 06 - Myoinositol Supplementation Helps Women Ovulate and Achieve Pregnancy with PCOS
- 07 - Should I take myoinositol in pregnancy with PCOS?
- 08 - Pregnancy induces a natural state of insulin resistance
- 09 - Metformin and Myoinositol
- 10 - Myoinositol use in Pregnancy to Avoid Gestational Diabetes Mellitus (GDM)
- 11- What have I seen in practice working with so many PCOS fertility and then PCOS pregnancy patients?
- 12- Should we consider myoinositol for mental health or sleep support?
- 13- What dosage of inositol is typically recommended?
- 14- What foods are a rich source of inositol?
- 15- THE BOTTOM LINE
- 16 - References
- 17 - DISCLAIMER
Spoiler alert. Yes! You can continue taking myoinositol in pregnancy.
In fact, myoinositol is something that helps many women with PCOS get pregnant. Naturally, they then ask “Should I keep taking this?”
My short answer is “yes”! Hang out with me for a bit of the “sciency” answer as to why.
Feel free to share this blog with your OB/GYN because I have seen too many doctors recommend their patients stop using this supplement during pregnancy. They have cited a lack of research, but I’m about to show you there is a clear frame of logic to continue taking it AND the research supports it too!
What is PCOS?
I asked this exact question when I was delivered my PCOS diagnosis. The doctor’s response: “PCOS is the number one leading cause of infertility in America.”
Thanks, doc, that’s not really what PCOS is. It’s a complex endocrine disorder with a misleading name. Its effect is system-wide, meaning your entire body feels the impact of PCOS.
PCOS actually stands for PolyCystic Ovarian Syndrome. It isn’t just about the ovaries. In fact, the ovaries are a downstream effect of endocrine challenges in a PCOS body. Without a great name, and without a doctor to actually help me (or you) understand this condition we have to turn to science.
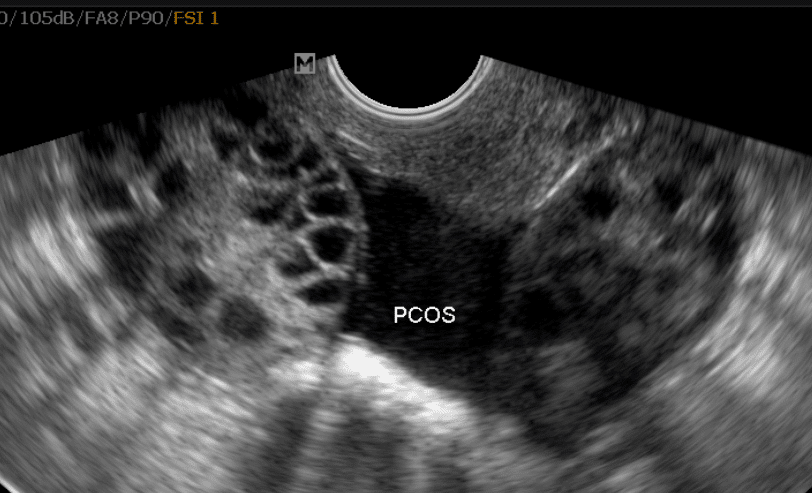
One of the most essential pieces for you to understand is there is an insulin signaling issue in the body of someone with PCOS. We require a lot of extra support to respond optimally to the hormone insulin.
Insulin signaling can make it more likely that you struggle with insulin resistance, but insulin resistance comes later. Insulin signaling inefficiencies can impact someone with PCOS that doesn’t have weight issues or insulin resistance.
What is insulin and why is it important to understand in the context of Polycystic Ovarian Syndrome?
Insulin is a hormone within the body. A hormone is simply a messenger that gets sent from one part of the body to another communicating something.
Insulin communicates this: Hey cell, energy is available, open up and take it in.
It also tells cells: If you have enough energy, store the extra for later. Making it a growth hormone.
It is widely known and understood that people with PCOS have a resistance to the message insulin sends.
When cells become resistant to insulin the body just creates more and more of it. It’s like turning up the volume when the message is having a hard time getting across. Ready for an illustration? Buckle your seat belts!
It’s the year 2004 and young 18 year old Caitlin is in Paris with her father and sister. They get in a taxi-cab.
This is before uber and before the ability to just put an address into your phone and point, or even have google translate for you. I’m really dating myself here.

In the cab my father gets in and says “we would like to go to the mall”. The cab driver had no idea what he was saying.
So what did my dad do?
He just turned up the volume and started shouting at the poor cab driver hoping that would help the message get through. “WE WOULD LIKE TO GO TO THE MALL”.
“These obnoxious Americans” the driver must have thought. This was my father’s solution to everything in another country where we didn’t speak the native language.
JUST GET LOUDER. Apparently, it’s your body’s first mode of operation too. Just pump out more insulin if the message isn’t getting across.
Oh, that didn’t do the job? Get louder body: MORE INSULIN!
Remember this example, because we are going to come back to it.
When cells become resistant to insulin our blood sugar levels rise. When blood sugar levels rise it can lead to inflammation and other issues.
Your body starts flooding more and more insulin(YELLING) from your pancreas to try and tell the rest of your body that ENERGY IS AVAILABLE.
Then there are unintended consequences. (hello androgens, weight gain, or in the context of pregnancy a “large for gestational age baby” and reactive hypoglycemia at birth for baby.
Want to learn more about inositol for PCOS? We have an entire article that is the ULTIMATE GUIDE to Inositol for PCOS, check out this article.
Your Ovary Doesn’t Become Insulin Resistant
While the rest of your body is struggling with high blood sugar levels the inside of your cells are starved for that sugar. Hello fatigue and brain fog. Yet your ovaries have something else going on.
So, when we talk about insulin resistance, it means that certain tissues in our body become less responsive to the effects of insulin. They are resistant to it.
Insulin is like a key that helps glucose (sugar) get into cells, where it’s used for energy. But in insulin resistance, some tissues start ignoring that key, making it harder for glucose to enter, and that can lead to high blood sugar levels.

There are some tissues in our body that don’t become insulin resistant. The good news is that our brain, eyes, and red blood cells don’t really develop insulin resistance. So, they keep responding to insulin as they should, allowing glucose to enter and do its job properly. Guess what other organ remains responsive: your ovary!
Well, that should sound like a good thing, but in PCOS it certainly is not.
When your ovary sees all that insulin it opens the doors so glucose molecules can shuttle inside the cell. When this happens the follicles within the ovary shift from making one of its primary hormones estrogen and instead start producing larger amounts of testosterone.
Cue the symptoms of PCOS including hair in unwanted areas, large polycystic ovaries, missed, irregular, or light periods, acne, hair loss, weight gain, dark skin patches, and infertility.(1)
The ovary goes into party mode when it is exposed to higher amounts of insulin. This isn’t the only thing at play though.
What is myoinositol?
Myoinositol is a vitamin like supplement that is part of the family of B vitamins and is also produced in the body starting from D-glucose.
Where does the term “myo” come into play? Most of inositol in its natural form is actually a “myo-inositol” isomer(a different shape of molecule).
“Myo-inositol” also represents the basis of something called “secondary messengers” and plays a huge part in processes including bone formation, reproduction and fertility, carbohydrate metabolism, and the functioning of nerves. (2)
Secondary insulin messengers, the ovary, and PCOS
A secondary messenger is a molecule that transmits a signal from the cell surface, where the insulin receptor is located, to the inside of the cell, where various cellular processes take place.
In other words, when insulin binds to its receptor on the cell surface, it initiates a series of events that ultimately lead to specific cellular actions, such as glucose uptake and metabolism.
Glucose uptake is just a fancy way of saying, bring the glucose from outside the cell, into the inside of the cell. Bring it form the blood outside to the inside of the cell to be used by things like the mitochondria.
The insulin signaling pathway is complex and involves a handful of secondary messengers, one of which is inositol.
Secondary messengers play a vital role in ensuring proper insulin responsiveness and glucose homeostasis in the body.
Let’s go back to the cab scenario.
My gentle-natured father becomes a yelling idiot in cabs with individuals who do not speak his language, we have established that.
Insulin acts similarly. It’s not getting the kids to the mall. So a secondary messenger is needed.
I pulled out my little English to French dictionary and looked up “Mall”. Digging deep to find my two years of high school French pronunciation I said “le centre commercial s’il vous plait”.
“Ahhhhh” the cab driver said. “Oui, oui.”
We needed a translator. The english, loud words weren’t getting the message across, we needed to translate it. THAT is exactly what the secondary messengers do.
Whelp! Guess what?! Women with PCOS have a bit of a disconnect with how these secondary signals work. (I know add insult to injury).
It’s as if you are in that same cab scenario, but even though you are in France you have a Spanish to English dictionary. Not as helpful!
We need more myoinositol to get the message across.

This is particularly important in the PCOS ovary.
One of the prominent studies that explored the imbalance of inositol metabolism in PCOS ovaries examined the levels of inositols in ovarian tissues of women with and without PCOS to compare us with ovaries who don’t have PCOS.
They found that in the ovaries of women with PCOS, there was an increase in the conversion of myo-nositol to D-chiro-inositol. (3)
We know from other research that D-chiro-inositol (the one we make too much of) is associated with an increase in the output of testosterone from the ovary.
We need more myoinsoitol to get the message insulin is sending to help protect the ovary. This can help it to do it’s job: make estrogen, instead of making more testosterone.
The imbalance of inositols in the ovaries is thought to contribute to the follicular and hormonal disturbances observed in PCOS, and it has led to the exploration of inositol supplementation as a potential therapeutic approach for PCOS management.
In particular, myoinositol supplementation has been studied and shows promise in improving ovulation and metabolic parameters in women with PCOS.
Myoinositol Supplementation Helps Women Ovulate and Achieve Pregnancy with PCOS
One of the reasons it can be so difficult to get pregnant with PCOS is related to the irregular nature or absence of ovulation. Myoinositol has been shown to lower testosterone levels, improve insulin resistance, and help stimulate ovulation.
By promoting regular ovulation, it increases the chances of conception in those who are trying to get pregnant. It also can help improve egg quality, which is essential for successful fertilization and embryo development.
Some studies have shown that myoinositol does not only assist with ovulation but also improves insulin sensitivity leading to better reproductive outcomes, less pregnancy risks, and more live births. And isn’t that the point anyways?
I have seen so many women conceive with the help of myoinositol supplementation. As with any medication or supplement, once you are pregnant, the next logical question is “should I stop taking this?”.

Should I take myoinositol in pregnancy with PCOS?
I know you already read the spoiler alert, but I want to frame a few things for you.
I was speaking with a naturopathic doctor a couple of years ago and we were discussing supplements that are helpful in assisting women with PCOS who are struggling with infertility get pregnant. Inositol came up and her response was:
“I love it when a supplement that helps someone get pregnant with PCOS is also a good fit to stay on in pregnancy. Then it doesn’t upset the system with a major change right after learning of the pregnancy.”
I often reflect on this comment because many medications and supplements that can be supportive for those struggling with fertility are not safe or recommended in pregnancy.

I can think of just a few that are. Magnesium comes to mind, vitamin D, and the star of this blog post: Myoinositol!
Myoinositol is something that helps insulin do its job in pregnancy. We need insulin to do its job, and especially for those of us with PCOS. Why?
Pregnancy induces a natural state of insulin resistance
PCOS is associated with hormonal imbalances and insulin resistance, which can affect the body’s ability to regulate blood sugar levels effectively.
During pregnancy, the body undergoes hormonal changes that can further impact insulin sensitivity(making it worse).
If a woman with PCOS becomes pregnant, the combination of pre-existing insulin resistance and pregnancy-related hormonal changes can increase the likelihood of developing gestational diabetes.
According to various studies and estimates, women with PCOS are approximately two to four times more likely to develop gestational diabetes compared to women without PCOS.
This increased risk is primarily attributed to the underlying insulin resistance that often accompanies PCOS.
Having a PCOS diagnosis alone increases the chances of gestational diabetes, so it’s very important to be proactive in managing blood sugar the best that you can.
There are many ways to approach management including adequate sleep, staying physically active, making intentional choices regarding diet strategies to impact blood sugar levels, and MEDICATIONS AND SUPPLEMENTS.
The most commonly used medication to help decrease risk or treat gestational diabetes mellitus is Metformin(or it’s generic form glucophage).
There is a shift in OBS and Midwives recommending metformin early in pregnancy to avoid Gestational diabetes that I have seen over the past few years, it is becoming more and more common.
Metformin is a prescription that has been used in an off-label manner to help treat PCOS. It helps address insulin resistance by reducing the liver’s glucose production and making the body’s cells more responsive to insulin.
It doesn’t increase insulin production but improves insulin’s effectiveness, which helps lower blood sugar levels and manage diabetes.
Some are prescribed metformin at diagnosis or are recommended its use to help stimulate ovulation or improve the effectiveness of ovulation stimulation medications.
It comes with significant side effects for some that include nausea and other GI disturbances like diarrhea.
When a woman is taking metformin to try and achieve pregnancy, she naturally comes to the same question, “should I stay on this in pregnancy?”
I am seeing physicians continuing to keep women on metformin in pregnancy in hopes to avoid gestational diabetes mellitus.

Metformin and Myoinositol
Both have sufficient research to conclude they help lower testosterone levels, improve insulin resistance, ovulation rates and even pregnancy rates.
However, myoinositol typically comes with less side effects and is a natural substance found in food and the human body.
Physicians that manage treatment of women for prenatal care and birth are more familiar with metformin, but that doesn’t make it superior.
How does myoinositol compare to metformin?
Myoinositol compared to metformin has 84% fewer side effects, and the same effect in lowering BMI, testosterone levels, improving glycemic outcomes, and regulating menstrual cycles.(4)
More specifically, there was a study conducted that included patients with PCOS taking metformin and inositol.
The study concluded that those with PCOS who were trying to conceive who took myoinositol and folic acid alone had a better ovulation and pregnancy rate compared to those who only took metformin alone.(4)
Myoinositol use in Pregnancy to Avoid Gestational Diabetes Mellitus (GDM)
In one study there was a 60% reduction in the development of Gestational Diabetes for those that took myoinsoitol compared with the placebo. (5)
When someone develops gestational diabetes mellitus they are more likely to have larger babies, need for insulin therapy, blood pressure disorders in pregnancy, preterm birth, and more interventions at the end of pregnancy to start labor.
Why wouldn’t someone want to take a supplement that could lower the risk of all those things?
In another study from January 2012 to December 2014, 220 pregnant women were randomized at two Italian University hospitals, 110 to myo-inositol and 110 to placebo.
The incidence of GDM was significantly lower in the myo-inositol group compared to the placebo group (11.6% versus 27.4%). Myo-inositol treatment was associated with a 67% risk reduction of developing GDM. (5)
What have I seen in practice working with so many PCOS fertility and then PCOS pregnancy patients?
Most western medicine providers have been trained in the use of medications instead of supplements and herbal treatments. It doesn’t make medication a wrong approach, but it doesn’t make it the best approach either.
I have worked with many hundreds of women who have focused their efforts on diet, exercise, and other lifestyle management factors in addition to taking myoinositol and I see much lower rates of GDM than even the study above that recorded 11.6% of those that took myoinositol went on to develop GDM.
Those that do go on to develop GDM who are taking myoinositol I see can usually manage the condition with the use of the supplement and lifestyle factors like movement and dietary strategies.
In fact, I will often increase the dosage of myoinsoitol after a diagnosis of Gestational Diabetes up form 4 gm per day to 6 gm per day.
There is so much that can be done with this supplement that often we don’t even need to enlist the help of metformin.
Should we consider myoinositol for mental health or sleep support?
If I’m asking the question you have got to believe there is a good answer.
Did you know that myoinositol can help you fall asleep? Have you heard of the mental health benefits of myoinositol?(6)
When it comes to pregnancy, especially a pregnancy that was fought for and hard to achieve with PCOS, mental health becomes a major concern.
Anxiety and depression are things we are more likely to experience without pregnancy, it makes sense that someone with PCOS might be entering pregnancy with a mental health or mood disorder and that it can only be heightened during pregnancy.
Supporting quality sleep and mental health become important objectives, and this one supplement can have application in these areas as well(a subject for another blog sometime).
What dosage of inositol is typically recommended?
Studies have shown that 4 grams per day for pregnant women is a sufficient dosage.
In women who have already been diagnosed with Gestational Diabetes I will at times increase the dosage up to a 6 gm per day with little side effects and improvements in glucose readings.
It is also important to consult with your care provider or doctor for further dosing education for your specific situation and pregnancy.
Can you take too much of myoinositol?
Yes, you can definitely take too much of anything. It is important to consult with your dietitian or healthcare provider about the correct dosage amount.
Higher doses of myoinositol have shown signs of nausea, headaches, dizziness, and fatigue. It is important that if you are experiencing these symptoms, especially during pregnancy, to contact your health care provider immediately.
What foods are a rich source of inositol?

Nervous to take a supplement while pregnant and would rather rely on food sources of myoinositol?
No problem! Food sources that contain myoinositol include:
- green beans
- peas
- asparagus
- walnuts
- grapes
- pears
- cherries
- apples
- tomatoes
- oats
- yeast
- carrots
While these foods contain myoinositol I have chosen to take and recommend others take supplemental form in pregnancy.
Why? To decrease the risk of developing Gestational Diabetes. You simply can not eat enough enough of these foods to get up to a 4,000 mg dose of myoinositol daily, so supplementing is prudent.
Did you notice that most of those foods that contain myoinositol also are foods that could spike your blood sugar. You may be increasing them for one benefit but actually increasing risk related to blood sugar issues, taking one step forward and steps backward.
I'm a dietitian, so I'm invested in "food first" approach 99% of the time, however when we are talking stakes as high as gestational diabetes in pregnancy and the risks that come along with it, I recommend and choose in my own pregnancies to be proactive and take myoinositol.
THE BOTTOM LINE
The bottom line is this: Studies have shown that myoinositol has been proven to increase the chances of fertility if you suffer from PCOS and has benefits that extend to pregnancy.
It has a very low risk profile and may help you avoid gestational diabetes. It can also be used to help treat gestational diabetes.
Why not use such a powerful and natural product to support your PCOS pregnancy?
If you are reading this and you are already pregnancy, I’m so happy for you and you’ve got this mama!
If you are reading this and still hoping to get pregnant, there is so much hope and we are here to support you too!
References
1 https://www.hopkinsmedicine.org/health/conditions-and-diseases/polycystic-ovary-syndrome-pcos
2 https://www.inositoli.it/en/myo-inositol/
4 A comparative study between myo-inositol and metformin in the treatment of insulin-resistant women
5 Myo-Inositol for the Prevention of Gestational Diabetes Mellitus. A Brief Review
6 Inositol treatment for psychological symptoms in Polycystic Ovary Syndrome women
DISCLAIMER
The advice provided in this article is for informational purposes only. It is not meant to augment and not replace consultation with a licensed health care provider. Consultation with a physician, dietitian, naturopathic doctor or other primary care provider is recommended for anyone suffering from a health problem.

I’M CAITLIN JOHNSON!
You are ready to trust your body again. You are ready to fix your hormones and fall in love with your body. Let me show you the way through comprehensive courses to manage your hormones and boost your fertility with PCOS.
Are you
struggling to get pregnant and you don’t know what step to take next. Join Find Fertility today and discover the process hundreds have used to get pregnant and have their dream baby.