at a glance
How is PCOS diagnosed?
What is PCOS?
PCOS, or polycystic ovarian syndrome, which was once seen as a gynecological disorder, is now better understood to be related to many metabolic processes and hormones. It is also a syndrome that matters beyond when a female is ready to have children or is frustrated with her menstrual cycle. There are hormonal abnormalities that are common with PCOS that tend to shift the “female hormones” like estrogen and progesterone so that they are created in smaller quantities and the “male hormones” or androgens are created in higher quantities.
This disorder affects a woman’s ability to reproduce and it ranks the number one reason women in the US struggle to have children.(1) In PCOS, follicles that are developing to eventually release an egg are halted in the process, primarily due to exposure to androgen excess(high levels of male hormones like testosterone). These follicles remain as fluid filled sacs on the outer edge of the ovary (2) and are the cysts that are present in PCOS.
Common Symptoms of PCOS:
Symptoms of polycystic ovary syndrome can feel very frustrating and may attack a woman’s vanity. PCOS symptoms range from facial hair to infertility. It may appear that these symptoms are only an attack on a woman’s self esteem and mental health. Yet, it’s not just about body hair falling out where she’d like to keep it (on the top of her head) or showing up where she’d like to remain smooth (chin, chest, neck, upper lip).
These symptoms are an evidence of underlying metabolic inefficiencies that have insidious outcomes like higher risk of heart disease and diabetes. As such it’s important to be able to recognize symptoms and obtain a proper diagnosis. There are some common PCOS symptoms you may be experiencing. (3)
Irregular periods
Increased facial and body hair
Difficulty with conception
Increased acne
Insulin resistance
Polycystic ovaries
Difficulty losing weight, or overall increased weight
Hair loss that is typically male patterned
Skin Tags
Dark or thick skin patches on the back of the neck, armpit area, and under breast tissue
How is PCOS Diagnosed?
So, you find yourself having a hard time losing weight, dealing with irregular periods, or struggling with fertility. You suspect something is up, you may even be thinking it’s probably PCOS, but now what?
The first step in getting a diagnosis is talking to your practitioner. Unfortunately, there isn’t a specific test to diagnose PCOS at this point, which is why you should be familiar with your symptoms when you speak to your practitioner. They will take a combined approach of listening to symptoms and health history, looking at lab markers, and performing additional testing like an ultrasound.
Which practitioner can diagnose PCOS?
Starting with a primary care physician(PCP) is always advised with any health concern. PCP are becoming more familiar with treating PCOS as it is now estimated to 6-12% of women of reproductive age. Since obstetricians and gynecologists(OB/GYNs) are typically the physician that is discussing a woman’s menstrual cycles with her the most they may be the first to suspect underlying hormonal issues and are likely the most common to diagnose PCOS.
Other specialists like dermatologists, endocrinologists and even reproductive endocrinologists may diagnose PCOS. While an endocrinologist is typically the doctor you think about treating “hormones” (and they are), you aren’t referred to an endocrinologist without a prior diagnosis of PCOS, thyroid disorders, or other hormonal abnormalities like diabetes that require treatment. Women that suffer from acne or suppurativa hidradenitis may have PCOS suggested as a root cause of the symptoms when consulting a dermatologist.
Naturopathic doctors are also a great source for diagnosing PCOS. Registered dietitians are often consulted by patients struggling with PCOS symptoms and while they can not diagnose PCOS, they can help provide referrals to other practitioners that have diagnosis as a part of their scope of practice.
Your primary care physician may ask you about your symptoms and recommend a blood test to test levels of male hormones like testosterone and DHEA-S. If they don’t, I recommend asking your physician for a blood test in order to specialize your treatment plan. I have a list of labs to request from your physician in a link here.
Other labs to request from your physician:
Checking for vitamin D levels and vitamin B12 levels are also worth testing at initial diagnosis.
Vitamin B12 becomes important if the doctor considers prescribing birth control or metformin as they both can deplete vitamin B12. These are the two most common prescriptions provided at diagnosis and both increase needs for vitamin B12. (4) This becomes even more important if someone is eating a diet low in meat and poultry.
Vitamin D is something that many are found to be deficient in. It is a vitamin, but it also has hormone-like qualities in the body and is a precursor to may sex hormones and thus it is incredibly important to check values and optimize levels.
What does getting diagnosed with PCOS look like?
After assessing your symptoms and health history your physician will likely order some labs to be drawn. The blood test will assess your levels of male hormones. It is helpful to request basic vitamin and metabolic tests too like: fasting blood sugar levels, and fasting glucose levels. (1) This way they can determine if your body has a normal response to glucose, or if there is an increased insulin spike.
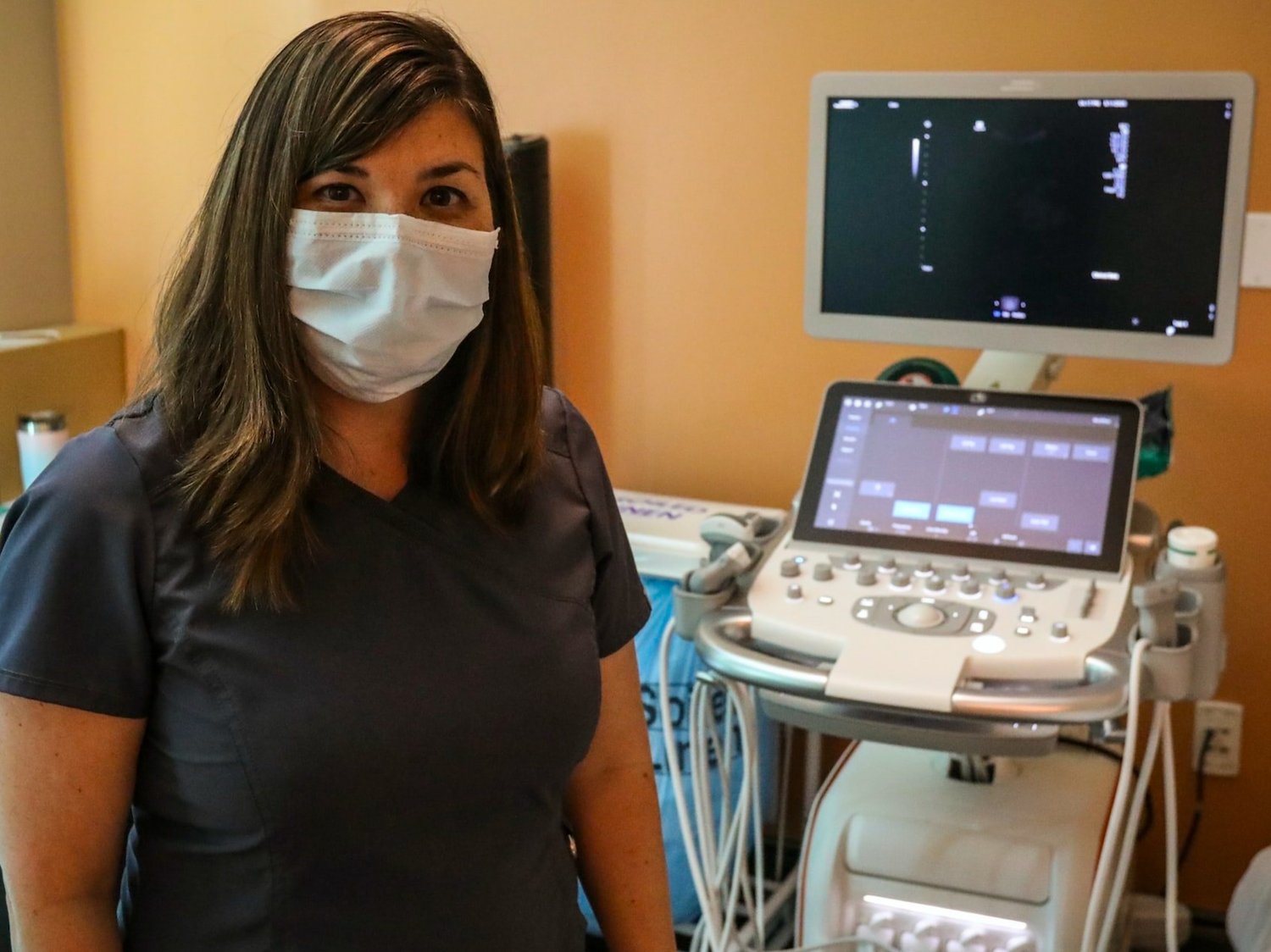
Your physician will also likely recommend an ultrasound. Typically a diagnostic ultrasound for PCOS is an internal ultrasound, so be prepared for that, I find many women are surprised when they show up to the appointment and would have preferred a heads up.(5)
You’ll need 2 out of the 3 to be diagnosed – The Rotterdam Criteria
Back in 2003 a group of PCOS experts all joined in a city in the Netherlands called Rotterdam. After much deliberation there was a consensus that was reached that helped guide diagnostic criteria for PCOS. This was actually a huge step forward because prior to this it was like the wild, wild west in terms of diagnosis (and honestly, sometimes it still is). So let’s chat about what these criteria are and some deviance I still see from doctor’s really coloring outside the lines.
Appearance of polycystic ovaries on an ultrasound
Lack of ovulation completely or irregular ovulation
Signs/symptoms or lab work with evidence of high levels of male hormones
It’s interesting that you only need two out of the three listed above to qualify for a diagnosis. The entire syndrome is named “Polycystic Ovarian Syndrome”, yet you don’t actually have to have polycystic ovaries to obtain the diagnosis. (6)

Even though there are estimates that 9 out of 10 women who have PCOS struggle with insulin resistance, doctor’s don’t typically look at insulin markers when diagnosing because of the Rotterdam criteria do not include them. Yet, if a patient doesn’t “appear” insulin resistant doctor’s may choose not to screen for PCOS. This can be frustrating for patients who have obvious symptoms but run into roadblocks on the medical side. Learning what the diagnostic criteria are, namely, The Rotterdam Criteria, can help you advocate for thorough testing and screening.
PCOS is a Diagnosis of Exclusion
There are many medical diagnosis’ that are not so cut and dry as test for this pathogen and call it the flu or looking at x-rays to determine if a bone has been broken. There is a lot of nuance and variables that have to be assessed for other conditions.
There is a large overlap of symptoms for which PCOS could be the cause or hypothyroidism could be the cause, namely hair loss, difficulty losing weight, infertility and cycle irregularities.
Another common condition that requires ruling out is a condition called non-classical congenital adrenal hyperplasia – this is something often diagnosed at birth or in childhood, but that increases androgen excess in the body and can lead to symptoms of high male sex hormones or infertility.
When we call something a diagnosis of exclusion it means that you have been assessed for these other conditions and they have been ruled out. During this process of ruling out these other conditions you are also being assessed for the diagnostic criteria for PCOS.
This can get a little confusing because it is actually possible to have both PCOS and hypothyroidism. There are other conditions that should also be excluded. See the list below for the most common.
hypothyroidism
hypothalamic amenorrhea (HA)
non-classical congenital adrenal hyperplasia (NCAH)
pituitary tumor
Should we even call it PCOS anymore?
There is an entire society called the “Androgen Excess & PCOS Society” that has proposed not only renaming the condition but considering removing the diagnostic criteria of having polycystic appearing ovaries.(7) This conversation needs to be considered in my opinion, but has little meaning in the scope of this blog post for you to be confident in your PCOS diagnosis.
What to do after diagnosis:
Once you are diagnosed with PCOS, you can start moving forward with a treatment plan. You can work individually with a PCOS dietitian or learn strategies related to nutrition in The PCOS App or one of my online courses.
Interventions can look very different based on your particular health goals, lab work and needs. It’s important to me you find comprehensive strategies that might include things like:
nutrition approaches
lifestyle changes
medications
exercise
supplementation
sleep quality
stress support
It is also important to remember that living with PCOS is not impossible. You may have to reframe your mindset around nutrition or movement, but it shouldn’t be a source of fear or worry. You can do it. Find a supportive community, work with a PCOS dietitian or practitioner, and remember, we are rooting for you. The PCOS App has on demand resources to enable you to improve your PCOS today.
1 https://www.womenshealth.gov/a-z-topics/infertility
2 https://www.mayoclinic.org/diseases-conditions/pcos/symptoms-causes/syc-20353439
3 https://americanpregnancy.org/womens-health/polycystic-ovary-syndrome
4 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3738982/
5 https://www.nichd.nih.gov/health/topics/pcos/conditioninfo/diagnose

I’M CAITLIN JOHNSON!
You are ready to trust your body again. You are ready to fix your hormones and fall in love with your body. Let me show you the way through comprehensive courses to manage your hormones and boost your fertility with PCOS.
Are you
struggling to get pregnant and you don’t know what step to take next. Join Find Fertility today and discover the process hundreds have used to get pregnant and have their dream baby.


